The facial nerve, formally known as Cranial Nerve VII (CN VII), is a vital and complex neurological structure. To psychologists, neuroscientists, and medical professionals, understanding the facial nerve is essential, as it forms the biological foundation of how we express human emotion. From a subtle frown to a radiant smile, the facial nerve orchestrates the intricate muscular movements that facilitate nonverbal communication.
This article provides a comprehensive overview of the facial nerve, detailing its anatomical pathway, primary functions, terminal branches, and the clinical consequences of its impairment.
Anatomy and Pathway of the Facial Nerve
The facial nerve is a mixed nerve, meaning it contains both motor and sensory fibers. Its anatomical journey from the brainstem to the face is highly complex and is generally divided into intracranial, intratemporal, and extracranial segments.
- Intracranial Origin: The nerve originates in the brainstem, specifically at the pontomedullary junction (the border between the pons and the medulla). It emerges as two distinct roots: a large motor root and a smaller sensory/parasympathetic root known as the nervus intermedius.
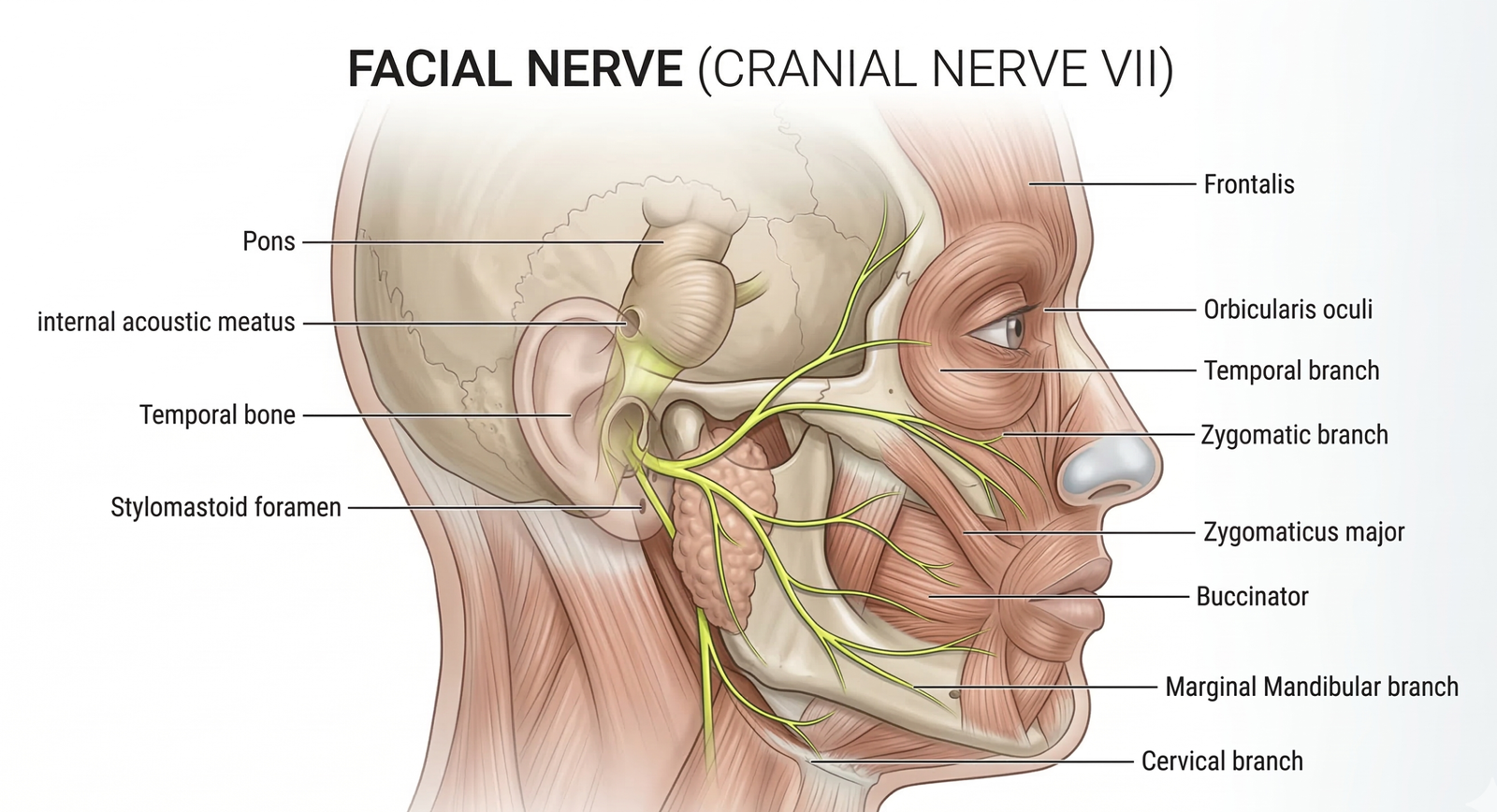
- Intratemporal Course: The nerve enters the temporal bone of the skull through the internal acoustic meatus. It then travels through a winding Z-shaped bony canal known as the facial canal. During this journey, it forms the geniculate ganglion, a collection of sensory neuron cell bodies.
- Extracranial Course: The nerve exits the skull through the stylomastoid foramen. Once outside the skull, the main motor trunk passes through the parotid gland (a major salivary gland in the cheek). It is vital to note that while the facial nerve passes through the parotid gland, it does not innervate it. Within the gland, the nerve divides into its five terminal branches.
Primary Functions
The facial nerve serves three distinct neurological functions, making it one of the most versatile cranial nerves in the human body.
1. Motor Function (Branchial Motor)
This is the most visually prominent function of CN VII. It provides motor innervation to the muscles of facial expression, including the frontalis (forehead), orbicularis oculi (around the eyes), and orbicularis oris (around the mouth). It also innervates the stapedius muscle in the middle ear, the posterior belly of the digastric muscle, and the stylohyoid muscle.
2. Sensory Function (Special Sensory)
The facial nerve is responsible for transmitting the special sense of taste from the anterior two-thirds of the tongue. These sensory fibers travel via a branch called the chorda tympani. It also provides a small area of general somatic sensation to the concha of the external ear.
3. Parasympathetic Function (Visceral Motor)
CN VII supplies parasympathetic (involuntary) innervation to several glands in the head. This includes the lacrimal glands (responsible for tear production) and the submandibular and sublingual glands (responsible for saliva production).
The Five Terminal Branches
After exiting the stylomastoid foramen and entering the parotid gland, the motor root of the facial nerve splits into five major terminal branches that spread across the face. Medical and psychology students often use the mnemonic “Ten Zebras Bit My Cheek” to remember them:
- Temporal Branch: Innervates the frontalis and orbicularis oculi muscles (allows for raising eyebrows and wrinkling the forehead).
- Zygomatic Branch: Innervates the lower part of the orbicularis oculi and muscles below the eye (facilitates closing the eyes tightly).
- Buccal Branch: Innervates the buccinator and upper lip muscles (aids in smiling, whistling, and keeping food in the mouth while chewing).
- Marginal Mandibular Branch: Innervates the muscles of the lower lip and chin (allows for depressing the lower lip, such as when pouting).
- Cervical Branch: Innervates the platysma muscle in the neck (draws the lower lip and corners of the mouth downward).
Clinical Significance and Disorders
Damage to the facial nerve can result in profound physical and psychological distress, severely impacting a patient’s ability to communicate emotion, eat, and protect their eyes.
Bell’s Palsy
Bell’s Palsy is the most common cause of acute facial nerve paralysis. It is an idiopathic (of unknown cause, though often linked to viral infections) lower motor neuron lesion. It results in sudden, unilateral (one-sided) weakness or paralysis of the entire half of the face. Patients may experience a drooping mouth, inability to close one eye, loss of taste, and hyperacusis (increased sensitivity to sound due to stapedius muscle paralysis).
Ramsay Hunt Syndrome
This condition occurs when the varicella-zoster virus (the virus that causes chickenpox and shingles) reactivates within the geniculate ganglion of the facial nerve. It causes facial paralysis similar to Bell’s Palsy, but is typically accompanied by a painful rash or blisters in the ear canal or mouth, and sometimes hearing loss or vertigo.
Diagnostic Nuance: Upper vs. Lower Motor Neuron Lesions
In neurology and biopsychology, assessing facial paralysis can help pinpoint the location of brain damage (such as from a stroke).
- Upper Motor Neuron Lesion (e.g., Stroke): Because the forehead receives bilateral motor input from the brain, an upper motor neuron lesion will paralyze the lower half of the face but spare the forehead. The patient can still raise both eyebrows.
- Lower Motor Neuron Lesion (e.g., Bell’s Palsy): A lesion at the nerve itself blocks all signals to that side of the face. The patient will experience paralysis of the entire half of the face, including the forehead.
Conclusion
The facial nerve is a complex superhighway of sensory, motor, and parasympathetic signals. For students and professionals in psychology, a deep understanding of Cranial Nerve VII is not just an exercise in neuroanatomy; it is fundamental to understanding the biological mechanics of human emotion, social signaling, and the psychological impact of facial motor disorders.