The study of consciousness in clinical psychology remains one of the most profound frontiers in understanding the human mind. For decades, researchers have grappled with the invisible mechanics of human awareness. However, this study is no longer confined to abstract academic debates. Today, understanding how the mind generates subjective experience is actively transforming how clinical psychologists treat severe cognitive and dissociative disorders.
This article explores how bridging the philosophical “hard problem” of consciousness with empirical clinical models offers groundbreaking pathways for psychological treatment.
The Philosophical Foundation: The “Hard Problem”
To understand the application of consciousness in clinical psychology, we must first look at the foundation laid by philosopher David Chalmers, who famously coined the “Hard Problem of Consciousness.”
Chalmers divided the study of consciousness into two categories:
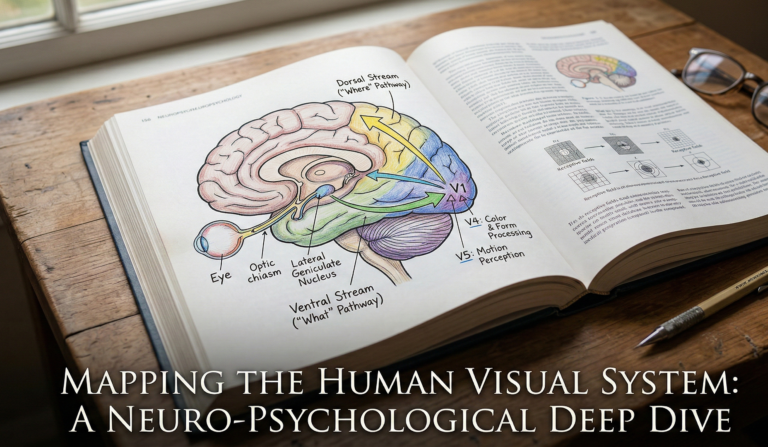
- The “Easy” Problems: These involve the mechanical and functional aspects of the brain. For example, how our eyes process light, how the brain integrates sensory data, or how we control our motor functions. Science can map these neurobiological processes.
- The “Hard” Problem: This asks why and how these physical processes give rise to subjective, inner experiences—often referred to as qualia.
A Practical Example: Imagine sitting on your porch, sipping a freshly brewed cup of coffee on a quiet morning. Neuroscientists can easily map the “easy problem”: the chemical receptors on your tongue reacting to the caffeine and transmitting signals to your brain. However, the “hard problem” is explaining the distinct, subjective feeling of warmth, comfort, and peace that you experience in that exact moment. Why does a biochemical reaction feel like anything at all?
When treating psychological disorders, clinicians must address both the “easy” neurological mechanics and the “hard” subjective suffering of the individual.
Key Theoretical Models of Consciousness
To bridge philosophy and empirical science, the field of consciousness in clinical psychology relies on several leading theoretical models to explain human awareness.
1. Global Workspace Theory (GWT)
Developed by Bernard Baars, GWT suggests that the brain operates like a theater. Unconscious processes take place in the dark, but when a piece of information needs attention, it is brought onto the brightly lit “stage” of the working memory, where it is broadcast to the rest of the brain.
2. Integrated Information Theory (IIT)
Proposed by Giulio Tononi, IIT takes a mathematical approach. It suggests that consciousness is a fundamental property of any complex, interconnected system. The more integrated and differentiated the information in a system (measured by a value called Phi), the more conscious it is.
3. Predictive Processing Model
This model argues that the brain is essentially a “prediction machine.” Rather than passively taking in the world, the brain constantly generates hypotheses about what will happen next based on past experiences. A Practical Example: Think about driving your usual route to the office. You often do this on “autopilot” because your brain perfectly predicts the environment. You only become acutely conscious of your surroundings when an “error” occurs—like a sudden road closure or a car abruptly braking in front of you.
Clinical Applications: When Consciousness Fragments
Understanding these models is vital when normal awareness breaks down, which is a primary focus when applying theories of consciousness in clinical psychology.
Dissociative Disorders
Conditions like Dissociative Identity Disorder (DID), Depersonalization, and Derealization involve a profound disruption in the normal integration of consciousness, memory, and identity.
- Through the lens of GWT: Dissociation can be viewed as a failure of the brain’s “broadcasting” system. Traumatic memories or certain identities are kept off the conscious “stage” and siloed in the dark unconscious, preventing the mind from experiencing a unified self.
- The Clinical Reality: An individual might feel entirely detached from their body during a high-stakes corporate meeting, feeling as though they are watching someone else speak their words. The subjective experience is deeply fractured.
Cognitive Processing Disorders
In conditions involving cognitive processing deficits (often seen in severe trauma, schizophrenia, or neurocognitive decline), the brain’s predictive processing models become rigid or flawed. The brain either hallucinates predictions without sensory input or fails to update its models when reality changes, leading to immense psychological distress.
Bridging the Gap: Empirical Clinical Treatments
How do clinicians use these theories to treat real-world suffering? The goal of modern treatment is to reintegrate the fragmented pieces of a patient’s conscious experience.
1. Somatic Experiencing and Grounding Techniques
To treat dissociation, clinicians must bridge the “hard problem” (the feeling of floating away or non-existence) with the “easy problem” (the body’s nervous system). Grounding techniques—such as touching a cold object, focusing on breathing, or engaging the senses—force the brain to update its predictive processing models by anchoring the patient into present, physical reality.
2. Mindfulness-Based Interventions
Mindfulness directly targets the Global Workspace. By training a patient to sit with their thoughts without judgment, clinicians help them bring suppressed, traumatic information back onto the “stage” of consciousness in a controlled, safe manner. This gradual exposure helps the brain process and integrate the trauma, reducing dissociative episodes.
3. Neurofeedback and Neuromodulation
Emerging treatments use neurofeedback to help patients visually see their brainwave activity (addressing the functional, easy problem) and learn to consciously regulate it. By bringing awareness to physiological states, patients with cognitive processing disorders can intentionally alter their subjective experiences of anxiety or detachment.
Conclusion
The philosophical “hard problem” of consciousness is not just an abstract debate; it is the lived reality of every patient seeking psychological help. Their subjective suffering is real. By understanding the theoretical models of how consciousness operates, clinical psychologists can develop highly targeted, empirical treatments. Bridging this gap allows the field of consciousness in clinical psychology to not only treat the neurological symptoms but to restore the unified, subjective experience of the human mind.