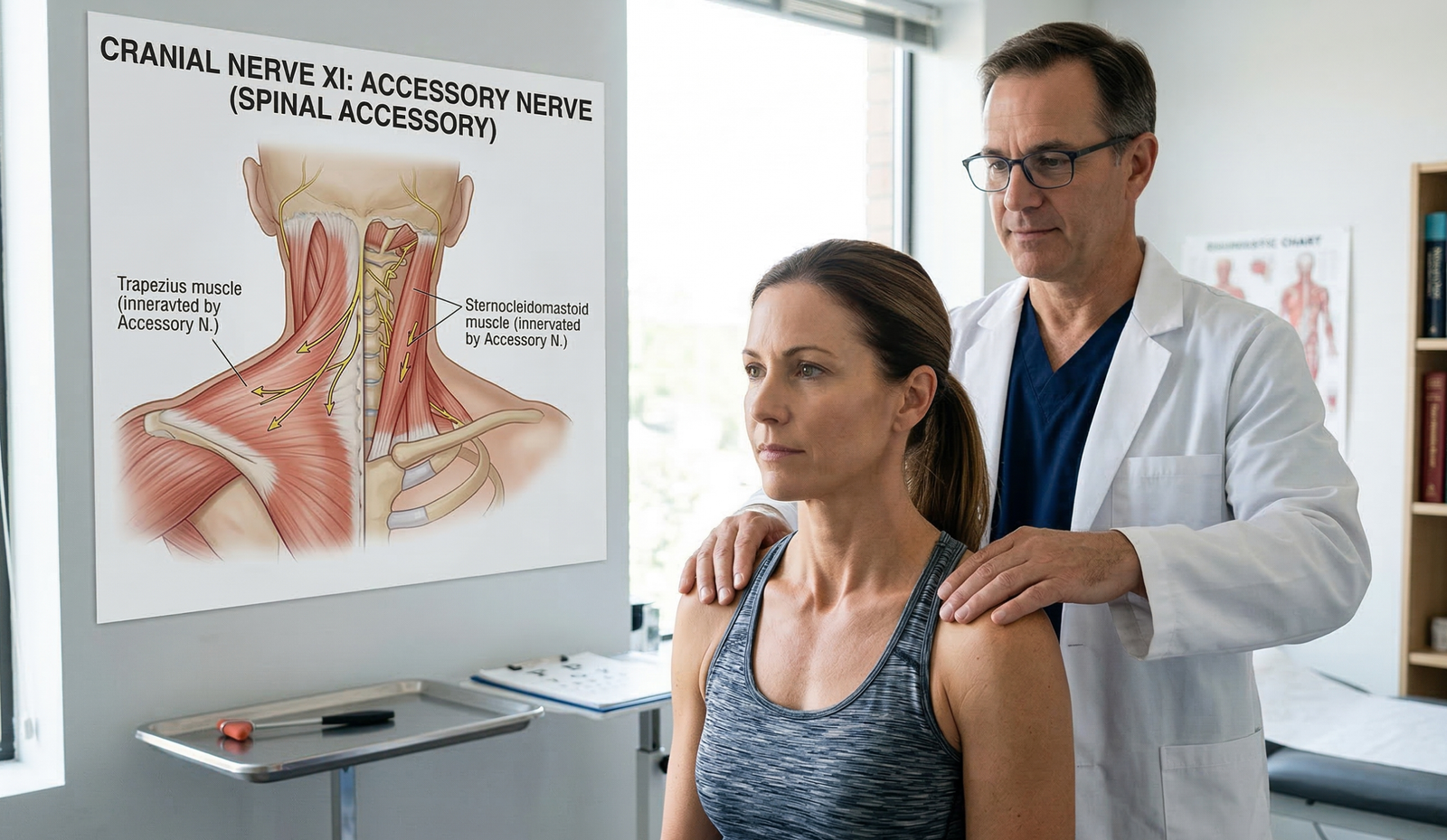
The human nervous system is a complex network that bridges the mind and the body, and the cranial nerves are essential to this communication. Among the twelve pairs of cranial nerves, the Accessory Nerve (Cranial Nerve XI)—often referred to as the spinal accessory nerve—holds a unique position. Unlike most cranial nerves that originate entirely within the brainstem, the accessory nerve possesses a distinct spinal origin.
Understanding the accessory nerve is vital for students of neuroanatomy, medical professionals, and neuropsychologists, as it governs key motor functions in the head, neck, and shoulders, and its impairment can lead to profound physical and somatic limitations.
1. What is the Accessory Nerve (CN XI)?
The accessory nerve is the eleventh cranial nerve (CN XI). It is primarily an efferent (motor) nerve, meaning it carries signals from the central nervous system outward to the muscles to initiate movement.
Historically, anatomists divided the accessory nerve into two parts: a spinal root and a cranial root. However, modern neuroanatomy increasingly views the cranial root as a structural component of the Vagus nerve (CN X). For clinical and practical purposes, when professionals discuss the accessory nerve, they are almost exclusively referring to the spinal accessory nerve.
2. Anatomy and Pathway
The pathway of the accessory nerve is distinct because it travels up into the skull before exiting it.
Origin
The nerve fibers originate from motor neurons in the upper spinal cord, specifically from segments C1 through C5 (and occasionally C6). These rootlets emerge from the spinal cord and merge to form a single nerve trunk.
Ascending and Exiting the Skull
Once formed, this trunk ascends and enters the skull through the foramen magnum (the large opening at the base of the skull). It briefly travels inside the cranium before turning back around to exit the skull alongside the glossopharyngeal (CN IX) and vagus (CN X) nerves through the jugular foramen.
Descent into the Neck
After exiting the skull, the spinal accessory nerve descends into the neck, traveling behind the internal jugular vein. It innervates the sternocleidomastoid muscle, crosses the posterior triangle of the neck, and finally terminates by innervating the trapezius muscle.
3. Primary Functions and Innervation
The accessory nerve provides exclusive somatic motor innervation to two major muscles:
- The Sternocleidomastoid (SCM): Located at the front and sides of the neck. When one side contracts, it allows the head to turn to the opposite side and tilt toward the same side. When both contract simultaneously, they flex the neck (bringing the chin to the chest).
- The Trapezius: A large, diamond-shaped muscle covering the upper back, shoulders, and back of the neck. The accessory nerve innervates the upper fibers of the trapezius, which are responsible for elevating the shoulders (shrugging) and rotating the scapula (shoulder blade) when raising the arm above the head.
4. Clinical Evaluation: How is CN XI Tested?
During a neurological exam, assessing the integrity of the accessory nerve is straightforward and relies on testing the strength of the SCM and trapezius muscles.
- Testing the Trapezius: The clinician asks the patient to shrug their shoulders upward while the clinician applies downward resistance. Weakness or asymmetry in the shrug indicates potential nerve impairment.
- Testing the Sternocleidomastoid: The patient is asked to turn their head to the left and then to the right against the resistance of the clinician’s hand placed on the patient’s cheek or jaw. If the nerve on the right side is damaged, the patient will have difficulty turning their head to the left.
5. Lesions and Damage: Spinal Accessory Nerve Palsy
Because of its superficial course through the posterior triangle of the neck, the accessory nerve is highly vulnerable to injury. Damage to this nerve is known as spinal accessory nerve palsy.
Common Causes of Injury
- Iatrogenic (Medical) Causes: The most frequent cause of damage is surgical intervention in the neck, particularly lymph node biopsies, tumor removals, or radical neck dissections.
- Trauma: Blunt force trauma, whiplash, or penetrating injuries to the lateral neck.
- Neurological Conditions: Though rare, conditions like tumors at the jugular foramen or motor neuron diseases can affect the nerve.
Symptoms of CN XI Palsy
Patients with a damaged accessory nerve typically present with:
- Shoulder drop: The affected shoulder rests visibly lower than the healthy one due to trapezius paralysis.
- Weakness in shrugging on the affected side.
- Difficulty raising the arm above shoulder level.
- Winged scapula: The shoulder blade protrudes outward when the arm is lifted laterally.
- Neck pain and shoulder aching: Often a result of other muscles overcompensating for the paralyzed trapezius.
6. Relevance to Psychology and Neuroscience
Why does a motor nerve matter in the context of psychology? The brain-body connection dictates that physical limitations deeply impact psychological well-being.
Patients suffering from iatrogenic accessory nerve damage often experience chronic pain, altered body image due to shoulder drooping, and an inability to perform daily tasks or jobs requiring overhead arm movement. This physical trauma frequently leads to comorbid psychological conditions, such as depression, anxiety, and a decrease in overall quality of life. Furthermore, from a psychosomatic perspective, the trapezius muscle (innervated by CN XI) is one of the primary sites where the human body holds psychological stress and tension.
Understanding the accessory nerve allows biopsychologists to appreciate the intricate mechanisms behind somatic symptom disorders, stress manifestation, and the holistic recovery process following neurological trauma.