When we examine the intricate relationship between human biology and psychology, the cranial nerves serve as the vital communication network between the brain and the external environment. Among these, the Abducens Nerve, or Cranial Nerve VI (CN VI), plays a highly specialized and indispensable role. While it is one of the smaller cranial nerves, its function is paramount to our visual perception and, consequently, how we interact with and interpret the world around us.
In this comprehensive guide, we will explore the neuroanatomy, primary functions, clinical pathologies, and neuropsychological implications of the abducens nerve.
What is the Abducens Nerve?
The abducens nerve is the sixth of the twelve cranial nerves. It is a purely somatic motor nerve, meaning its sole responsibility is to provide motor innervation to a specific voluntary muscle. The term “abducens” is derived from its primary function: it controls the abduction of the eye, which is the movement of the eye away from the midline of the face (looking outward toward the ear).
Neuroanatomy and Pathway
Understanding the pathway of the abducens nerve is crucial for neurologists and neuropsychologists when localizing lesions or diagnosing the root cause of ocular motor deficits. The nerve takes a long and complex anatomical journey:
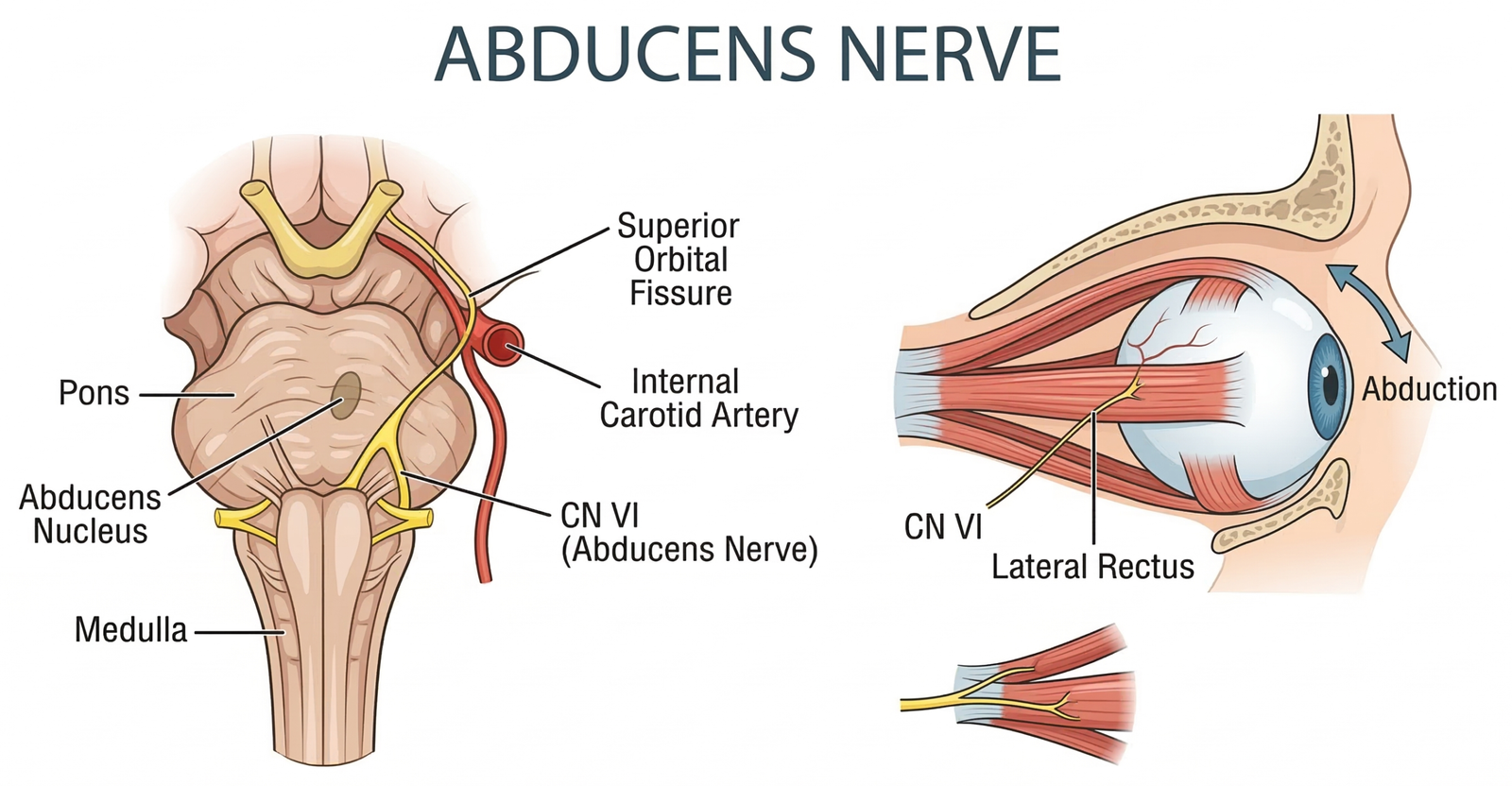
- Origin (The Abducens Nucleus): The nerve originates in the abducens nucleus, located in the lower portion of the pons (part of the brainstem), just beneath the floor of the fourth ventricle.
- Exit from the Brainstem: The nerve fibers travel anteriorly and exit the brainstem at the pontomedullary junction (the division between the pons and the medulla oblongata).
- The Subarachnoid Space: Upon exiting, it travels upward through the subarachnoid space, running along the clivus. This segment makes the nerve particularly vulnerable to downward pressure from increased intracranial pressure (ICP).
- The Cavernous Sinus: The nerve pierces the dura mater and enters Dorello’s canal, eventually traveling through the cavernous sinus alongside the internal carotid artery.
- Termination: Finally, it enters the bony orbit of the eye through the superior orbital fissure, terminating at the lateral rectus muscle.
Primary Function: Controlling the Lateral Rectus Muscle
The functional scope of the abducens nerve is singular yet essential. It innervates the lateral rectus muscle of the ipsilateral (same side) eye.
- Lateral Gaze: When the lateral rectus muscle contracts, it pulls the pupil away from the nose. If you want to look to your right, the right abducens nerve activates the right lateral rectus muscle to pull the right eye outward.
- Binocular Vision: The abducens nerve does not work in isolation. The abducens nucleus contains interneurons that connect to the contralateral (opposite side) oculomotor nerve (CN III) via the medial longitudinal fasciculus (MLF). This ensures that when one eye looks outward, the other eye simultaneously looks inward, allowing for coordinated, binocular vision.
Clinical Significance: Abducens Nerve Palsy
When the abducens nerve is damaged or compressed, it results in a condition known as Abducens Nerve Palsy (or Sixth Nerve Palsy). Because of the nerve’s long intracranial course, it is highly susceptible to injury.
Common Symptoms
- Horizontal Diplopia: Patients typically experience double vision that worsens when looking toward the affected side.
- Esotropia (Medial Strabismus): Because the lateral rectus muscle is paralyzed, the medial rectus muscle operates unopposed, pulling the affected eye inward toward the nose.
- Compensatory Head Posture: Patients may frequently turn their head toward the side of the paralyzed eye to minimize double vision.
Common Causes
The etiology of CN VI palsy can vary widely depending on the patient’s age and overall health:
- Microvascular Disease: Conditions like diabetes mellitus and hypertension can compromise blood flow to the nerve. This is the most common cause in older adults.
- Trauma: Head injuries can stretch or tear the nerve.
- Increased Intracranial Pressure (ICP): Tumors, hydrocephalus, or idiopathic intracranial hypertension can compress the nerve against the clivus. This is often considered a “false-localizing sign,” as the pathology may not be near the nerve itself.
- Infections and Inflammation: Meningitis, viral infections, or conditions like multiple sclerosis.
Neuropsychological and Psychological Implications
While the abducens nerve is structurally a motor nerve, the psychological fallout of its dysfunction can be profound. From a neuropsychological perspective, visual processing is fundamental to cognitive assessment and daily functioning.
- Impact on Cognitive Testing: Many standardized neuropsychological assessments rely heavily on visual stimuli. Uncorrected diplopia resulting from CN VI palsy can severely skew test results, masquerading as cognitive impairment, poor attention, or processing speed deficits.
- Psychological Distress: Sudden onset of double vision is highly distressing. It impairs reading, driving, and spatial navigation, often leading to a loss of independence. This can precipitate acute anxiety, social withdrawal, and depressive symptoms in patients.
- Visual Processing and Perception: The brain requires congruent information from both eyes to construct a stable representation of the world. Disruption to the abducens nerve forces the brain to either adapt to the double vision or suppress the image from the affected eye, an adaptation that requires significant cognitive load.
Conclusion
The abducens nerve is a testament to the specialized architecture of the human nervous system. Though it controls only a single muscle, its integrity is essential for coordinated vision and spatial interaction. For professionals in the field of psychology and neuropsychology, understanding the mechanics and vulnerabilities of Cranial Nerve VI provides crucial context for evaluating visual processing, diagnosing neurological anomalies, and providing empathetic care to patients navigating the psychological distress of visual impairment.